Tacrolimus Dose Adjustment Calculator
Calculate Your Tacrolimus Adjustment
Results will appear here
When someone gets a kidney, liver, or lung transplant, they’re given tacrolimus to stop their body from rejecting the new organ. It works. But here’s the problem: if they get a fungal infection-something common after transplants-and are put on an azole antifungal like voriconazole or itraconazole, their tacrolimus levels can skyrocket overnight. And when that happens, their kidneys start to fail. This isn’t rare. It’s routine. And it’s preventable.
Why Azoles and Tacrolimus Don’t Mix
Tacrolimus is broken down in your liver by enzymes called CYP3A4 and CYP3A5. Think of them like trash disposals. Azole antifungals? They’re like jamming a stick into that disposal. They block the enzymes. So tacrolimus doesn’t get cleared. It builds up. And fast.Studies show that ketoconazole can push tacrolimus levels up by 300% to 500%. Voriconazole? Usually 100% to 300%. Even posaconazole, often seen as "safer," can still double or triple levels. The result? Blood concentrations that go from a safe 6-10 ng/mL to 18-30 ng/mL or higher. And at those levels, toxicity isn’t a risk-it’s a guarantee.
Here’s what happens next: your kidneys tighten up. Blood flow drops. Creatinine spikes. You get acute kidney injury. Some patients need dialysis. Others lose the transplant. And because the symptoms-fatigue, swelling, less urine-are easy to miss, it often gets caught too late.
The Real Cost: Nephrotoxicity in Transplant Patients
Nephrotoxicity from tacrolimus isn’t just a side effect. It’s a leading cause of long-term kidney damage in transplant recipients. One study from Johns Hopkins found that 15-20% of all tacrolimus-related kidney injuries were directly tied to azole interactions. That’s not a fluke. That’s a pattern.And it’s not just about the drug. It’s about timing. When a transplant patient starts an azole, their tacrolimus level isn’t checked for days. Sometimes not until they’re already in the ER. A patient on the American Transplant Foundation forum shared: "My levels jumped from 6.5 to 18.2 in one night. My creatinine doubled. I was in the hospital for a week." That’s not an outlier. It’s the norm in clinics without protocols.
Even worse? The damage isn’t always reversible. Chronic kidney disease can develop months later. And once it does, the patient’s long-term survival drops-not from rejection, but from kidney failure.
Not All Azoles Are Created Equal
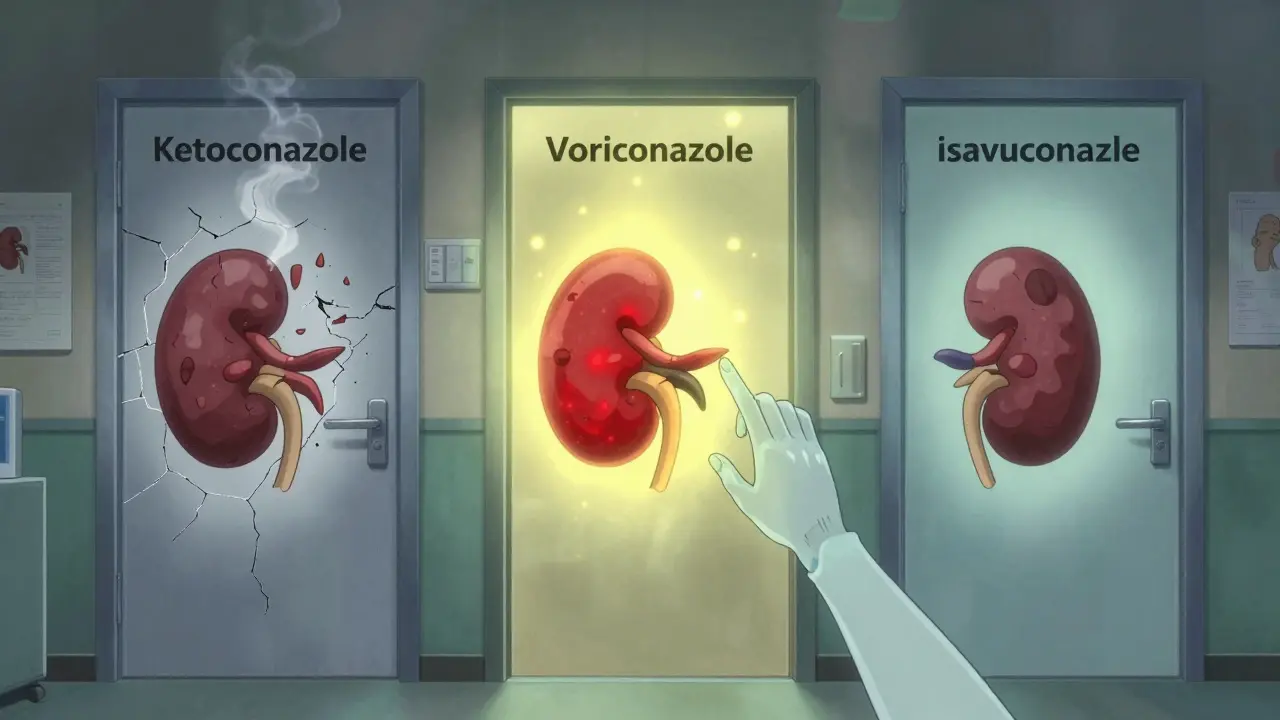
Some azoles are worse than others. Ketoconazole? It’s the worst offender. Strongest CYP3A4 blocker. Almost never used anymore, but it still pops up in older prescriptions or in countries with less regulation.Voriconazole? Common in lung transplant patients. It’s great for aspergillosis. But it’s also the top reason for tacrolimus spikes in transplant centers. One pharmacist on Reddit said: "We see this weekly. We start posaconazole, and within 72 hours, tacrolimus is through the roof."
Then there’s isavuconazole. It’s newer. And it’s quieter. It barely touches CYP3A4. Studies show it only raises tacrolimus levels by 30-50%. That’s manageable. But here’s the catch: insurance often won’t cover it. It’s more expensive. So even though it’s safer, many patients still get the riskier drugs.
And then there are the alternatives: echinocandins like micafungin, or lipid amphotericin B. They don’t mess with CYP3A4 at all. But they’re IV-only. They’re harder to give long-term. And amphotericin B? It can hurt your kidneys on its own. So now you’re trading one toxin for another.
What Clinicians Do-And What They Should Be Doing
The best transplant centers have protocols. They don’t guess. They don’t wait. When an azole is added:- Tacrolimus dose is cut by 50-75% for voriconazole or ketoconazole.
- For posaconazole, it’s 25-50%.
- For isavuconazole? Maybe 10-20%.
And then? Daily blood tests for the first five days. Then three times a week until stable. That’s not optional. That’s standard. But not every center does it.
A 2022 survey of 127 transplant pharmacists found 89% said azole-tacrolimus interactions were the most common dangerous interaction they managed. And 76% said these interactions led to at least one unplanned hospital admission every month in their unit.
Why? Because many hospitals still don’t have automated alerts in their electronic records. No one remembers. No one checks. The patient goes home on a new antifungal, and the tacrolimus dose stays the same. Two days later, they’re back in the ER.
What You Can Do-If You’re a Patient or Caregiver
If you’re on tacrolimus and your doctor says you need an antifungal:- Ask: "Which one? Is there a safer option?"
- Ask: "Will my dose change? By how much?"
- Ask: "How often will my blood be checked?"
- Know the signs: less urine, swollen ankles, extreme fatigue, nausea, confusion.
- Don’t wait for symptoms. If you’re on an azole, assume your tacrolimus is too high until proven otherwise.
Some patients have been told, "We’ll just monitor." But monitoring without dose adjustment is like checking your car’s oil level after the engine’s already seized.

The Bigger Picture: Why This Keeps Happening
There are 42,857 transplants in the U.S. every year. That’s a lot of people on tacrolimus. And nearly half of them get antifungals-especially lung and liver recipients. So this isn’t a niche issue. It’s a systemic one.Guidelines exist. The American Society of Transplantation says avoid strong CYP3A4 inhibitors. They say reduce tacrolimus by 50-75%. But implementation? Patchy. One transplant center reduced toxicity by 60% after they started cutting tacrolimus by 75% when starting posaconazole. That’s huge. But only 78% of centers have any protocol at all.
And now, there’s new hope: extended-release tacrolimus. It smooths out peaks and valleys in blood levels. Early data suggests it might reduce kidney damage by 22%. And research into CYP3A5 genetics? That could mean future dosing based on your DNA. But that’s still years away.
Right now, the solution is simple: reduce the dose. Check the levels. Don’t wait.
What’s Next?
The field is moving. More centers are using C/D ratios (concentration per dose) instead of just trough levels. That’s smarter. It accounts for how fast your body processes the drug. And more antifungals are being studied-like olorofim-that won’t touch CYP3A4 at all.But until then, the rule is clear: if you’re on tacrolimus and need an azole, assume you’re one step away from kidney failure. Don’t rely on luck. Don’t rely on memory. Use the protocol. Ask the questions. Push for the right drug. Your transplant-and your kidneys-depend on it.
Can azoles cause permanent kidney damage in transplant patients?
Yes. When azoles spike tacrolimus levels, they can trigger acute kidney injury that doesn’t fully reverse. Repeated episodes or prolonged high levels can lead to chronic kidney disease, reducing long-term transplant survival. Studies show that up to 15% of tacrolimus-related kidney damage in transplant patients is directly linked to azole interactions.
Is there a safer antifungal than voriconazole for transplant patients on tacrolimus?
Yes. Isavuconazole is the safest azole option-it only raises tacrolimus levels by 30-50% on average. Echinocandins like micafungin and caspofungin don’t interact with CYP3A4 at all, making them ideal for IV use. Lipid-formulation amphotericin B is another alternative, though it carries its own kidney risk. The key is matching the drug to the patient’s risk level and availability.
How often should tacrolimus levels be checked when starting an azole?
Daily for the first 3-5 days after starting the azole. After that, check at least 2-3 times per week until levels stabilize. Some centers use continuous monitoring with C/D ratios (concentration per dose) for better accuracy. Waiting longer than 72 hours without checking is a common cause of severe toxicity.
Why do some doctors still use ketoconazole with tacrolimus?
They shouldn’t. Ketoconazole is the strongest CYP3A4 inhibitor and has been largely replaced due to its high toxicity risk. But in some regions or older treatment plans, it’s still prescribed because it’s cheap or available. Major guidelines now explicitly warn against its use with tacrolimus. If you’re on ketoconazole with tacrolimus, ask for an alternative immediately.
Can switching to a different immunosuppressant avoid this interaction?
Yes. Belatacept is a non-CNI immunosuppressant that doesn’t rely on CYP3A4 metabolism, so it has no interaction with azoles. It’s approved for kidney transplant patients and is being used more often, especially in those with frequent infections. But it’s not used for liver or lung transplants yet, and it requires IV infusions. For now, CNI-based regimens like tacrolimus remain standard-but awareness of alternatives is growing.